Plantar fasciitis

What are the symptoms of plantar fasciitis?
Typical comments from patients with debilitating heel pain might be:
- “It feels like I’ve been stabbed in the heel with a hot poker.”
- “I get a stabbing pain in my heel when I get up in the morning. It usually improves after a few minutes of limping around.”
- “After sitting for a while, when I stand up the stabbing pain returns.”
- “I dread putting my feet on the ground in the morning and walk around on my toes to stop the pain.”
Why is plantar fasciitis called heel spur?
Plantar fasciitis is most commonly described as a ‘heel spur’ or ‘heel pain’ which often, but not always, occurs in the morning.
The plantar fascia or Achilles tendon is a tendon that runs under the foot from the heel (calcaneus) to all five toes.
Heel spurs occur over time from stresses to the tendon which pulls on the bone, causing calcification and forming the spur. It is not the spur itself that causes the pain, but where the tendon attaches to the bone. This becomes inflamed and causes the pain, with or without associated other soft tissue involvement. Around 60% of people with spurs have no symptoms.
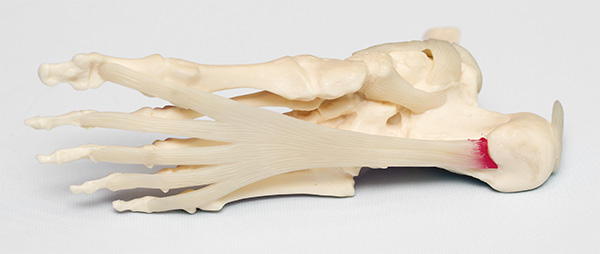
What brings on plantar fasciitis?
Causes include weight gain, tight calf muscles, pronation (rolling in of the foot) and supination (rolling out). An increase in frequency of exercise, poor footwear or age can also inflame the plantar fascia tendon.
How does a podiatrist diagnose heel spur?
An ultrasound differentiates the thickness of the plantar fascia and can determine the presence of a fascial tear in which case it will need to be treated and offloaded with a moonboot. However an ultrasound is not always required.
How does a podiatrist treat heel pain?
Wearing appropriate footwear is important in mitigating heel pain, in particular avoiding thongs or ballet flats as much as possible. As our podiatrists focus on biomechanics, we are experts in shoe recommendation.
Orthotic therapy – the prescription of customised foot orthotics – is the single most effective treatment for this type of condition.
Stretching will also assist along with decreasing the frequency of exercise until inflammation subsides. Massaging the tendon by rolling your foot over a ball (such as a tennis ball or speciality massage ball) can help stimulate the healing process, however, this is quite painful.
Other solutions may involve:
- Rest
- Cold presses or ice packs
- Anti-inflammatory tablets
- Cushioning
- Massaging the foot
- Muscle strengthening
- Stretching exercises
Strapping, with or without heel raises, by your podiatrist is highly recommended to correct the foot position and allow the plantar fascia to heal. A qualified podiatrist will assess the right treatment for each individual case.
Healing time varies widely on a case-by-case basis. In the worst-case scenario the plantar fascia has torn or ruptured. The quicker heel pain is treated, the better the outcome will be.
Could it be something other than plantar fasciitis?
There are other possible conditions: fractured calcaneus, baxters nerve entrapment, bursitis, achilles tendonpathy, tibialis posterior dysfunction, or particularly Sever’s Disease in children. However plantar fasciitis is the most common heel condition.



